A world first! my country achieves regenerated islet transplantation, opening a new path for diabetes treatment.
March 18, 2026
Source: drugdu
 131
131
Reporters learned from the Center for Excellence in Molecular Cell Science (Institute of Biochemistry and Cell Biology), Chinese Academy of Sciences, that Professor Cheng Xin's research group at the center, in collaboration with Professor Yin Hao's team at the Second Affiliated Hospital of Naval Medical University (Shanghai Changzheng Hospital), recently achieved, for the first time internationally, minimally invasive transplantation of regenerated islets (E-islets) derived from autologous and allogeneic stem cells, enabling pancreatic islet function reconstruction and autonomous blood glucose regulation in patients with type 1 diabetes. The relevant findings have been published online in the international academic journal *The Lancet Diabetes & Endocrinology*.
Diabetes is a chronic disease that seriously threatens the health of Chinese residents, with type 1 diabetes being most prevalent in children and adolescents. Due to autoimmune disorders and the body's immune system's abnormal attack and destruction of pancreatic beta cells, pancreatic function fails, insulin secretion is severely insufficient, and blood sugar is difficult to control. It has long been considered an irreversible chronic disease. Patients must rely on insulin injections and frequent blood glucose monitoring for life, enduring not only the physical and mental stress of long-term treatment but also the potential for serious complications such as kidney failure, blindness, cardiovascular and cerebrovascular damage, hypoglycemic coma, and even death, threatening their lives and health. While traditional islet transplantation is effective, it is limited by a severe shortage of donors, preventing its accessibility to a large number of patients. How to achieve large-scale regeneration of islet tissue has become a pressing problem for the global medical community.
After more than 20 years of in-depth research, a Chinese research team has established a brand-new technical system based on endoderm stem cells and successfully constructed "regenerated islet E-islet" for the treatment of severely impaired pancreatic islet function and type 2 diabetes. After being infused into the patient via the portal vein, regenerated islet E-islet can function like normal pancreatic tissue, maintaining stable blood glucose control.
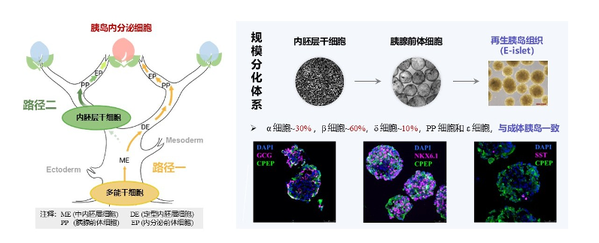 In vitro pancreatic islet reconstruction technology based on endoderm stem cells
In vitro pancreatic islet reconstruction technology based on endoderm stem cells
The research team conducted clinical trials in three patients using E-islets derived from autologous or allogeneic endoderm stem cells, evaluating efficacy and safety under different immunosuppressive strategies. Through these clinical studies, the team demonstrated for the first time internationally that both autologous and allogeneic regenerated islet transplantation can achieve islet function reconstruction, autonomous glycemic regulation, and exogenous insulin withdrawal in patients with type 1 diabetes, thereby improving long-term glycemic levels and effectively reducing the occurrence and progression of complications. However, this therapy currently requires combination with long-term immunosuppressive therapy to overcome issues such as autoimmune relapse in type 1 diabetes.
In the future, the research team will further modify the regenerated islets through gene editing and other means, making them no longer recognized by the immune system, thereby avoiding the use of immunosuppressants and ultimately achieving the goal of completely curing diabetes.
https://www.guancha.cn/industry-science/2026_03_17_810427.shtml
By editorRead more on
- Boehringer Ingelheim’s new oral drug “Zonaitinib” has been approved for a new indication in China May 22, 2026
- Class 1 innovative drug Fazanleisen tablets approved May 22, 2026
- Shijiazhuang Pharmaceutical Group’s budesonide enteric-coated capsules approved! This poses a challenge to generic drug manufacturers, weakening the original drug’s competitive advantage. May 22, 2026
- Two world-first drugs from Chipscreen Biosciences have been launched in the Macau market, further improving patient accessibility! May 22, 2026
- Beimei Prostol Eye Drops Receives Drug Registration Certificate May 22, 2026
your submission has already been received.
OK
Subscribe
Please enter a valid Email address!
Submit
The most relevant industry news & insight will be sent to you every two weeks.



