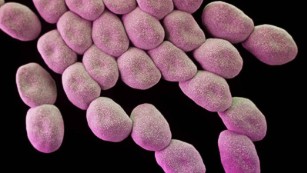
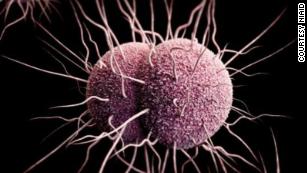
Among the priority pathogens is a drug-resistant tuberculosis, which kills about 250,000 people around the world each year, and a variety of multidrug resistant strains -- Acinetobacter, Pseudomonas and various Enterobacteriaceae -- which are responsible for infections in hospitals and nursing homes and among patients whose care requires ventilators and catheters.
Of the 33 potential medicines for treating priority bug infections, only eight are innovative treatments. The other 25 are simple modifications of existing families of antibiotics. At best, then, the 25 will serve as short-term solutions since it is expected bacteria will quickly adapt to and resist these new (though somewhat familiar) drugs, according to the WHO.
"It is difficult to speculate why companies develop specific new medicines," Beyer noted. "But in general many new treatments do not necessarily constitute advances over existing treatments."
TB infections require a combination of at least three antibiotics, according to the new report, yet only seven of the new TB medicines are even in clinical trials. Soon, there will be a serious lack of treatment options for this infection, the report warns.
The same is true for gram-negative pathogens, which can cause severe, often deadly infections typically in hospitals and nursing homes.
Gram-negative bacteria have more complex cell walls than gram-positive, explained Beyer. "In a nutshell, it is more complex to develop a novel antibiotic that can penetrate the complex gram-negative cell wall and stay inside the bacterium," he wrote.
Finally, the WHO sees too few oral antibiotics being developed. These are necessary "to target the critical priority pathogens (and) be accessible in low- and middle-income countries," Beyer noted.
To address the problem of developing new antibiotics, the WHO and the Drugs for Neglected Diseases Initiative set up the Global Antibiotic Research and Development Partnership. However, new drugs alone cannot combat the threat of antimicrobial resistance. The WHO is also working to improve infection prevention and control while developing guidance for the responsible use of antibiotics.
"Always seek medical advice before taking antibiotics and then always follow the advice of the health-care professional," Beyer noted.
The new report is a "fantastic (and very useful!) summary" of the antibiotic situation, wrote Bill Hanage, an associate professor of epidemiology at Harvard T.H. Chan School of Public Health, in an email. Hanage, who has also published studies of antibiotic resistance, was not involved in the new report.
Although the risk of getting a completely resistant infection is low in the United States, about 2 million people each year become infected with "resistant enough" bacteria that are harder to treat, Hanage said. And every year, more than 20,000 people die of these infections.
"More resistant infections don't just mean you or someone you care about is more likely to die from one, they also mean healthcare will get even more expensive," Hanage said. "Many of the procedures we take for granted in medicine, from cancer treatments to surgeries, depend on our ability to handle infections that happen in the course of treatment."
The number of new drugs in development is simply not enough, he said.
"The great majority will not make it into the hands of doctors or your treatment," Hanage wrote. "As the report states, for drugs to be used in humans they have to pass 3 hurdles, the phase 1, 2 and 3 trials. Drugs entering that pipeline have just a 14% chance of getting all the way through to be used in humans."
Copyright©2026 Ddu. All rights reserved.
 1,054
1,054